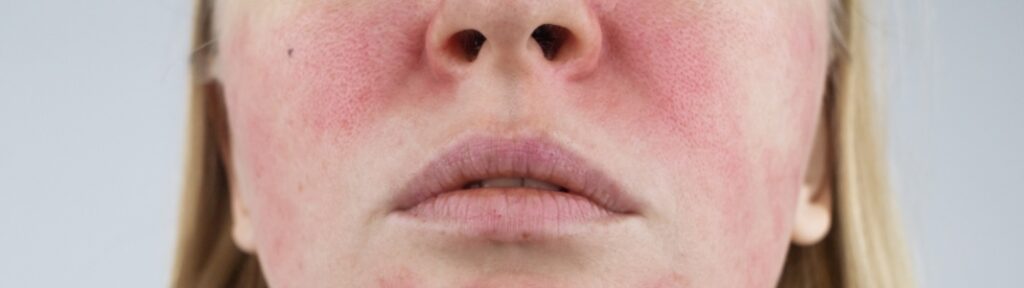
Rosacea (pronounced "roh-ZAY-sha") is a chronic and potentially life-disruptive disorder primarily of the facial skin, often characterized by flare-ups and remissions. Many have observed that it typically begins any time after age 30 as a redness on the cheeks, nose, chin or forehead that may come and go. In some cases, rosacea may also occur on the neck, chest, scalp or ears. Over time, the redness tends to become ruddier and more persistent, and visible blood vessels may appear. Left untreated, bumps and pimples often develop, and in severe cases the nose may grow swollen and bumpy from excess tissue. This is the condition, called rhinophyma (pronounced "rhi-no-FY-muh"), that gave the late comedian W.C. Fields his trademark bulbous nose. In many rosacea patients, the eyes are also affected, feeling irritated and appearing watery or bloodshot.
What Should I Look For?
Rosacea can vary substantially from one individual to another, and in most cases some rather than all of the potential signs and symptoms appear. According to a consensus committee and review panel of 17 medical experts worldwide (see Classification of Rosacea), rosacea always includes at least one of the following primary signs, and various secondary signs and symptoms may also develop.
Primary Signs of Rosacea
Flushing
Many people with rosacea have a history of frequent blushing or flushing. This facial redness may come and go, and is often the earliest sign of the disorder.
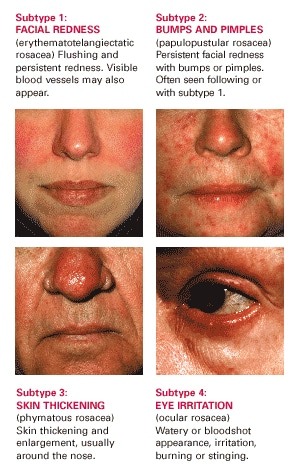
Persistent Redness
Persistent facial redness is the most common individual sign of rosacea, and may resemble a blush or sunburn that does not go away.
Bumps and Pimples
Small red solid bumps or pus-filled pimples often develop. While these may resemble acne, blackheads are absent and burning or stinging may occur.
Visible Blood Vessels
In many people with rosacea, small blood vessels become visible on the skin.
Redness (erythema)
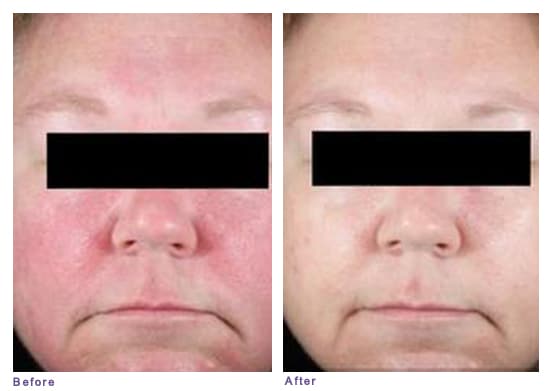
Patient with Subtype 1 (erythematotelangiectatic) rosacea, before and after treatment with topical gel.
Bumps (papules) and Pimples (pustules)
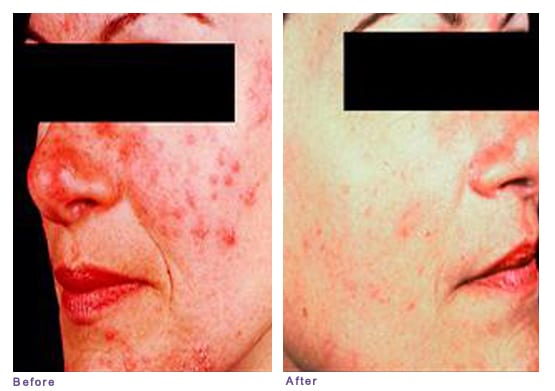
Patient with Subtype 2 (papulopustular) rosacea, treated with topical therapy in a split-face study.
Visible Blood Vessels (telangiectasia)
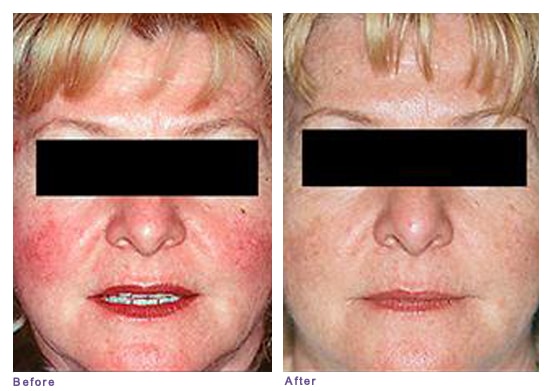
Patient with Subtype 1 (erythematotelangiectatic) rosacea, before and after pulsed-dye laser treatment.
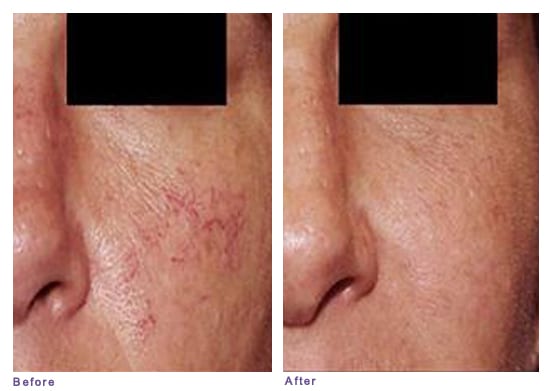
Patient with Subtype 1 (erythematotelangiectatic) rosacea, before and after treatment with a pulsed-dye laser
Want Beautiful, Clear Skin?
It starts here. Come see us today!